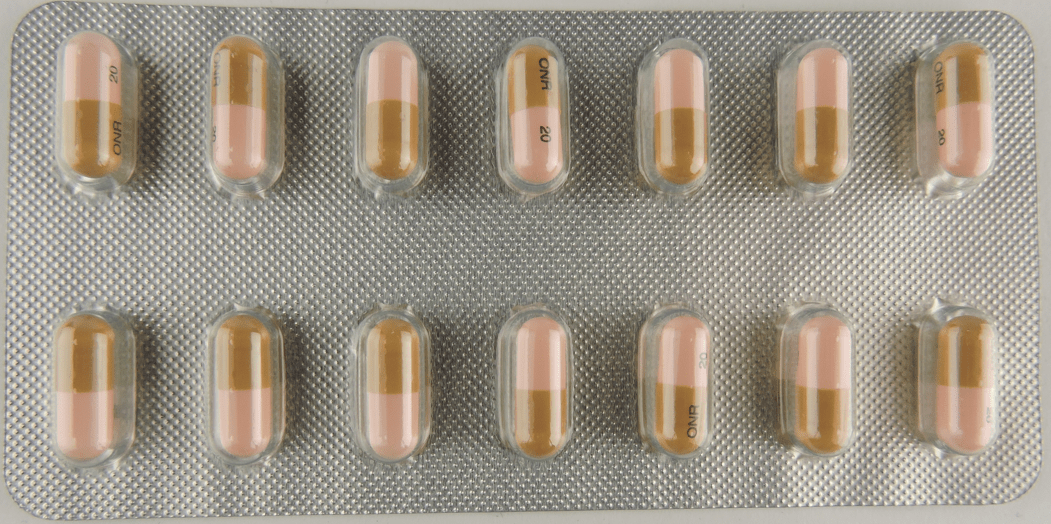
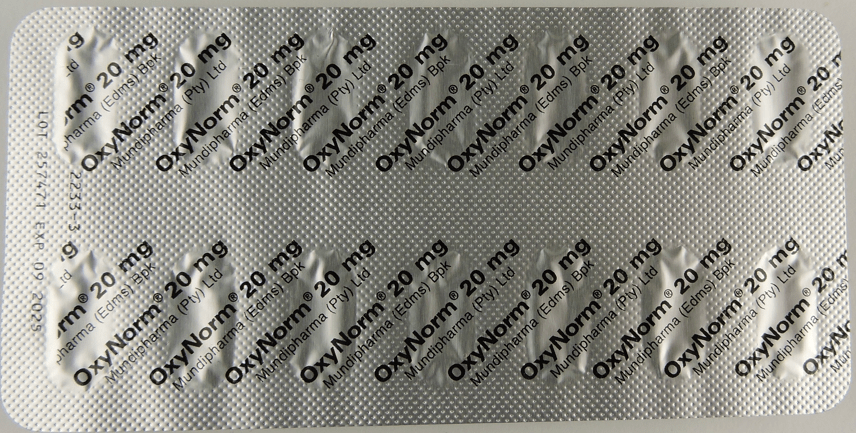
OxyNorm (Oxycodone) 20mg – 28caps
$215
OxyContin is a brand-name version of the extended-release form of Oxycodone. They are different versions of the same drug. OxyContin and immediate-release oxycodone belong to a drug class called opioids. A class of drugs is a group of medications that work in a similar way and are often used to treat similar conditions. Immediate-release oxycodone and OxyContin both bind to receptors in your brain and spinal cord. When they do this, they block pain signals and stop pain.
In stock
Description
WARNING – MAY BE HABIT FORMING
OxyContin is a brand-name version of the extended-release form of Oxycodone. They are different versions of the same drug. OxyContin and immediate-release oxycodone belong to a drug class called opioids. A class of drugs is a group of medications that work in a similar way and are often used to treat similar conditions. Immediate-release oxycodone and OxyContin both bind to receptors in your brain and spinal cord. When they do this, they block pain signals and stop pain.
Immediate-release Oxycodone is a powerful pain reliever. It is highly effective at treating pain.
This drug is a very powerful pain reliever. It is important to know everything you can about this drug before you take them. It can be habit forming, even at low doses and when taken exactly as prescribed. Misuse of this drug can lead to addiction, poisoning, overdose, or even death. If you are prescribed this drug, it’s very important that you talk to your doctor about how to use this drug safely.
Usual Adult Dose for Chronic Pain
The following dosing recommendations can only be considered suggested approaches to what is actually a series of clinical decisions over time
60 and 80 mg extended-release (ER) tablets, a single dose greater than 40 mg (36 mg oxycodone base), a total daily dose greater than 80 mg (72 mg oxycodone base), or use of the 100 mg/5 mL (20 mg/mL) oral solution should be restricted to use in opioid-tolerant patients only.
- Initial dose for OPIOID-NAIVE patients: 5 to 15 mg orally every 4 to 6 hours on an around-the-clock basis
- Oral solution: To avoid dosing errors total dose should be included in both mg and mL
MAINTENANCE: Adjust dose every 1 to 2 days as needed to obtain an appropriate balance between pain management and opioid-related adverse reactions; goal should be to find the lowest effective dosage for the shortest duration consistent with individual patient treatment goals
Do not take OxyNorm capsules if you:
- are allergic (hypersensitive) to oxycodone, or any of the other ingredients of the capsules;
- have breathing problems, such as severe chronic obstructive lung disease, severe bronchial asthma or severe respiratory depression. Your doctor will have told you if you have any of these conditions. Symptoms may include breathlessness, coughing or breathing more slowly or weakly than expected;
- have a condition where the small bowel does not work properly (paralytic ileus), your stomach empties more slowly than it should (delayed gastric emptying) or you have severe pain in your abdomen;
- have a heart problem after long-term lung disease (cor pulmonale);
- have increased carbon dioxide levels in the blood. Symptoms may include dizziness, drowsiness, fatigue, shortness of breath and headache;
- have moderate to severe liver problems. If you have other long-term liver problems you should only take these capsules if recommended by your doctor;
- have ongoing problems with constipation;
- are under 18 years of age.
Warnings and precautions
Talk to your doctor or pharmacist before taking these capsules if you:
- or anyone in your family are or have ever been addicted to opioids, alcohol, prescription medicines or illegal drugs;
- are a smoker
- have ever had problems with your mood (depression, anxiety or a personality disorder) or have been treated by a psychiatrist for other mental illnesses);
- have previously suffered from withdrawal symptoms such as agitation, anxiety, shaking or sweating, when you have stopped taking alcohol or drugs;
- feel you need to take more capsules to get the same level of pain relief, this may mean you are becoming tolerant to the effects of this medicine or are becoming addicted to it. Speak to your prescriber who will discuss your treatment and may change your dose or switch you to an alternative pain reliever;
- are elderly or weakened;
- have an under-active thyroid gland (hypothyroidism), as you may need a lower dose;
- have myxoedema (a thyroid disorder associated with dryness, coldness and swelling or puffiness of the skin affecting the face and limbs);
- know you are suffering from a brain injury or tumour, or you have a head injury, severe headache or feel sick, as this may indicate that the pressure in your skull is increased;
- have low blood pressure (hypotension);
- have low blood volume (hypovolaemia). This can occur due to severe external or internal bleeding, severe burns, excessive sweating, severe diarrhoea or vomiting;
- feel very lightheaded or faint;
- have a mental disorder following use of certain medicines (toxic psychosis);
- have inflammation of the pancreas (which causes severe pain in the abdomen and back);
- have problems with your gall bladder or bile duct;
- have inflammatory bowel disease;
- have an enlarged prostate gland, which causes difficulty in passing urine (in men);
- have poor adrenal gland function (your adrenal gland is not working properly which may cause symptoms including weakness, weight loss, dizziness, feeling or being sick), for example due to Addison’s disease;
- have severely impaired lung function. Symptoms may include breathlessness and coughing;
- have long term pain unrelated to cancer;
- have a condition where your breathing stops for short periods whilst you are asleep, known as sleep apnoea;
- have kidney or liver problems.
Taking this medicine regularly, particularly for a long time, can lead to addiction and may result in life threatening overdose. If you have concerns that you may become dependent on OxyNorm capsules, it is important that you consult your doctor. Your doctor should have explained how long you will be using it for and when it is appropriate to stop, how to do this safely.
Rarely, increasing the dose of this medicine can make you more sensitive to pain. If this happens, you need to speak to your doctor about your treatment.
Addiction can cause withdrawal symptoms when you stop taking this medicine. Withdrawal symptoms can include restlessness, difficulty sleeping, irritability, agitation, anxiety, feeling your heartbeat (palpitations), increased blood pressure, feeling or being sick, diarrhoea, loss of appetite, shaking, shivering or sweating. Your doctor will discuss with you how to gradually reduce your dose before stopping the medicine. It is important that you do not stop taking the medicine suddenly as you will be more likely to experience withdrawal symptoms.
Opioids should only be used by those they are prescribed for. Do not give your medicine to anyone else. Taking higher doses or more frequent doses of opioid may increase the risk of addiction. Overuse and misuse can lead to overdose and/or death.